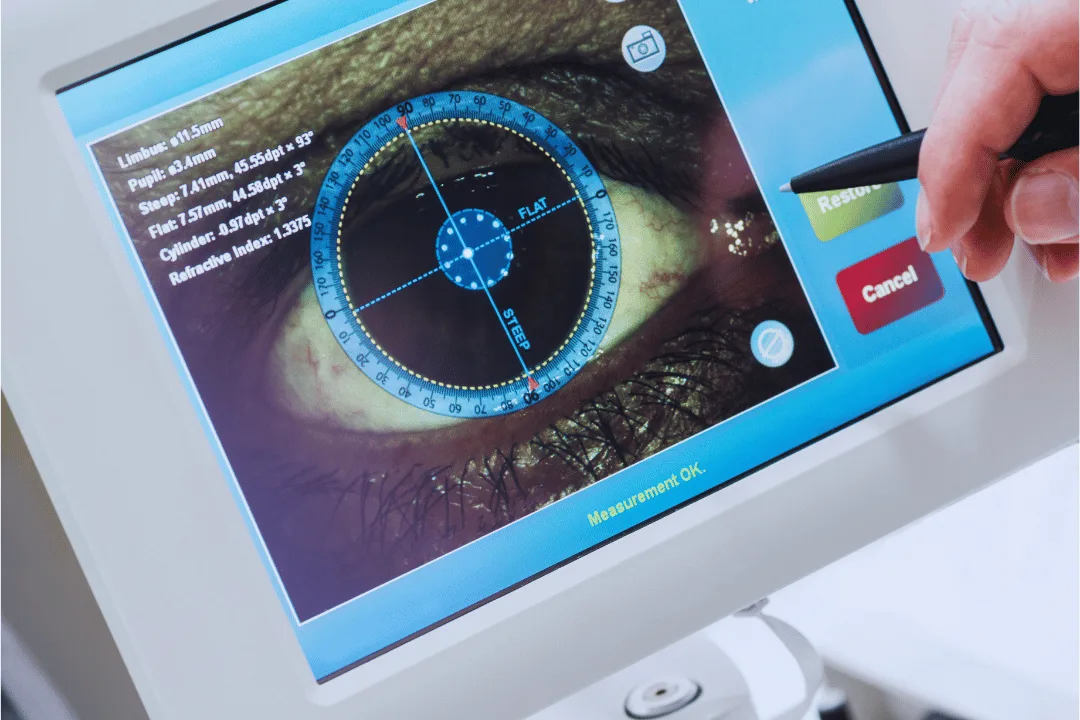
Artificial intelligence (AI) is making waves in healthcare, transforming how doctors diagnose and treat diseases. In a recent study, a team of scientists explored a fascinating new area called oculomics—an innovative field where AI analyzes images of the eye to find clues about diseases in other parts of the body. By focusing on the retina, the light-sensitive layer at the back of the eye, this research aims to provide a window into a person’s overall health, particularly for conditions like diabetes and cardiovascular disease.
At the heart of this research is a method that uses AI to detect HbA1c levels, a marker of blood sugar control that is crucial in diagnosing and managing diabetes. Typically, doctors measure HbA1c levels through a blood test, but this new approach uses a non-invasive eye scan to get the same information. This breakthrough has the potential to make diabetes screening faster, easier, and more accessible to millions of people worldwide, especially in communities where regular healthcare isn’t readily available.
Joshua Ong, one of the lead researchers, emphasizes just how powerful this new technology can be. “AI and oculomics give us a glimpse of how non-invasive tools can make life-saving screenings more accessible, especially in underserved areas. The ability to assess something as critical as HbA1c through an eye image could really change the game for early detection,” he explains. Imagine visiting your optometrist for a routine eye exam and, at the same time, getting screened for diabetes without even a needleprick. This kind of dual-purpose test could be a huge convenience, and more importantly, it could save lives by identifying diseases earlier.
So, how does it all work?
The research team used thousands of retinal images from patients, both with and without diabetes, and fed them into a machine-learning algorithm. In simple terms, the AI “learns” to recognize patterns in these images that are linked to different levels of HbA1c. The images were categorized based on whether the patients had normal blood sugar levels, pre-diabetes, or diabetes. Over time, the AI became more skilled at making these distinctions, reaching an accuracy rate of about 60-62%—an encouraging start for a new technology that is still in development.
But it’s not just about the technology itself; it’s also about making sure this tool is trustworthy and reliable. Lead scientist Insup Lee points out that for AI to be trusted in medical settings, it needs to be as transparent as possible. “Doctors and patients need to trust that the AI is making accurate and fair decisions, especially when it comes to something as important as diagnosing diabetes,” he says. In their study, the researchers didn’t just measure the AI’s accuracy; they also focused on potential biases in the system. For instance, they found that the AI performed differently depending on the patient’s age and gender. This kind of variation, if not addressed, could lead to misdiagnoses.
The researchers discovered that younger patients—especially those under 50—tended to have higher HbA1c levels than older patients, likely because younger individuals often have Type 1 diabetes, which is more difficult to control. Additionally, the AI appeared to behave differently when analyzing retinal images from men versus women. Interestingly, when trained on a mixed dataset of both men and women, the AI was more accurate across the board. This finding highlights the importance of having diverse data when training AI, ensuring it performs well for everyone, not just specific groups.
These challenges underline a bigger question about AI in healthcare: How do we ensure that this technology works for all patients, regardless of age, gender, or ethnicity? Lee stresses that this is a crucial area for future research. “We need to continuously improve the diversity of the data that AI models are trained on to avoid biases and ensure fair treatment for all patients,” he explains. In other words, AI can only be as good as the data we feed it. The more varied and representative that data is, the better the AI will be at diagnosing diseases in all types of people.
Looking forward, the team has high hopes for how this technology could evolve. While the current models are still in their early stages and not yet accurate enough for clinical use, the researchers are optimistic about future improvements. “With more data, better algorithms, and ongoing fine-tuning, we believe AI could one day match or even surpass traditional methods for measuring HbA1c,” says Kuk Jin Jang, another lead researcher. This is an exciting prospect, especially when you consider how widespread diabetes is becoming around the world. By 2030, it’s expected that over 550 million people will be living with diabetes globally. With such a high number of people at risk, having a quick, easy, and non-invasive way to screen for this disease could be a real game-changer.
Moreover, the potential uses for AI in oculomics extend beyond diabetes. The eye can reveal so much more than just eye-related conditions. As this technology develops, it could be used to screen for cardiovascular disease, neurodegenerative conditions like Alzheimer’s, and even cancers. This means that one eye exam could provide a wealth of information about your overall health.
As Ong puts it, “We’re just scratching the surface of what’s possible with AI in healthcare. The future looks bright, and it’s closer than we think.”
For more information on this groundbreaking research, you can explore the full study conducted by Joshua Ong, Insup Lee, Kuk Jin Jang, and their team. Visit: https://doi.org/10.1016/j.apjo.2024.100095